Does Medicaid Cover GLP-1 Drugs? A State-by-State Guide (2026 Update)
Key Takeaways
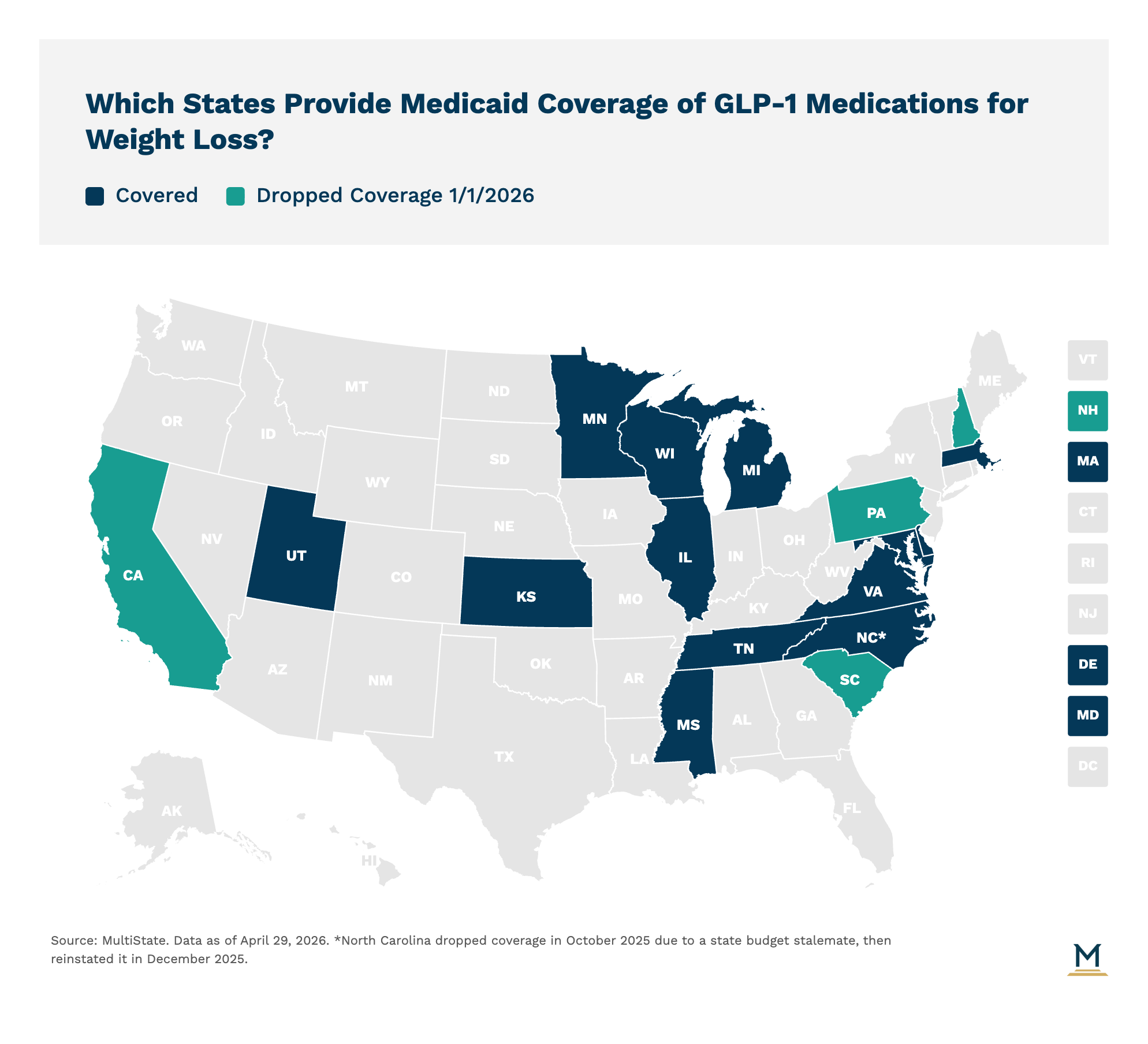
- As of early 2026, only 13 state Medicaid programs cover GLP-1 medications like Ozempic, Wegovy, and Zepbound for weight loss, down from 17 states at the start of the year. California, New Hampshire, Pennsylvania, and South Carolina dropped their state Medicaid GLP-1 coverage in January 2026, citing budget constraints from the high cost of these medications.
- Even in states with Medicaid obesity medication coverage, access requires meeting strict criteria like BMI thresholds over 30, prior authorization, and documented failure with traditional weight loss programs first. The CMS BALANCE model launching in May 2026 could expand GLP-1 weight loss Medicaid access through negotiated manufacturer pricing, though state participation is voluntary.
- State GLP-1 policy 2026 reflects growing tension between demand for these medications and their budget impact, with some states also removing coverage from employee health plans separate from their Medicaid programs.
Which States Cover GLP-1 Medications for Weight Loss in 2026?
As of early 2026, only 13 state Medicaid programs cover GLP-1 medications specifically for weight loss, including Ozempic, Wegovy, and Zepbound. Coverage remains fairly restrictive and has contracted sharply since the start of the year: prior to January 1, 2026, a total of 17 states offered this coverage. It is worth noting that this post addresses coverage for obesity and weight loss only. Most state Medicaid programs are required to cover GLP-1 medications when prescribed for Type 2 diabetes, which is a separate coverage category under federal Medicaid rules.
Recent State Coverage Cuts and Budget Pressures
The reduction in weight loss coverage is attributable to decisions made by four states (California, New Hampshire, Pennsylvania, and South Carolina) that discontinued their coverage. The primary justification cited by these states for cutting this benefit was budgetary constraints, highlighting the substantial cost pressure these popular, high-priced medications place on state health budgets. Colorado, North Carolina, and West Virginia made similar decisions to remove GLP-1 medications for weight loss from their state employee health plans, though this is distinct from their Medicaid programs.
Access Requirements and Restrictions for Medicaid GLP-1 Coverage
Even in the 13 states that maintain coverage, access is not guaranteed and is subject to stringent utilization management (UM) parameters designed to limit use to the most severe cases and control costs. These measures ensure that the drugs are prescribed only after less expensive, traditional interventions have failed. Common restrictions include:
BMI Thresholds for Eligibility
Enrollees typically must have a body mass index (BMI) over 30 (the standard definition for obesity) to qualify for the medication. Some states may also require a BMI over 27 with certain obesity-related comorbidities.
Prior Authorization and Step Therapy Requirements
Patients are frequently required to undergo a process known as "step therapy," meaning they must first demonstrate failure with other, often non-pharmaceutical, weight loss programs or less expensive treatments (such as diet and exercise programs, or older, cheaper weight loss medications) before a GLP-1 can be approved.
Documentation Requirements for Prescribers
Prescribers must usually provide clear documentation that the enrollee has actively participated in and failed to achieve clinically meaningful weight loss through these prerequisite programs.
Colorado’s Medicaid program does not cover GLP-1 drugs for weight loss. The state also removed these medications from its state employee health plan, joining North Carolina and West Virginia in doing so. These decisions reflect the same budget pressure driving Medicaid policy changes nationally, though state employee benefit decisions are made separately from Medicaid coverage policy.
Federal Policy Changes and the CMS BALANCE Model
The federal policy picture is shifting. CMS has introduced the BALANCE model, a demonstration program that would allow state Medicaid agencies to expand GLP-1 coverage for obesity beginning as early as May 2026 through negotiated manufacturer pricing. Participation is voluntary for states, so the impact on Medicaid coverage will vary. A KFF analysis tracks state-level Medicaid coverage and spending on GLP-1s and is updated as state policies change.
Complete State-by-State Medicaid GLP-1 Coverage Chart
| State | Medicaid Coverage for Weight Loss |
|---|---|
| Alabama | No coverage |
| Alaska | No coverage |
| Arizona | No coverage |
| Arkansas | No coverage |
| California | Dropped coverage 1/1/2026 |
| Colorado | No coverage |
| Connecticut | No coverage |
| Delaware | Has coverage |
| District of Columbia | No coverage |
| Florida | No coverage |
| Georgia | No coverage |
| Hawaii | No coverage |
| Idaho | No coverage |
| Illinois | No coverage |
| Indiana | No coverage |
| Iowa | No coverage |
| Kansas | Has coverage |
| Kentucky | No coverage |
| Louisiana | No coverage |
| Maine | No coverage |
| Maryland | Has coverage |
| Massachusetts | Has coverage |
| Michigan | Has coverage |
| Minnesota | Has coverage |
| Mississippi | Has coverage |
| Missouri | No coverage |
| Montana | No coverage |
| Nebraska | No coverage |
| Nevada | No coverage |
| New Hampshire | Dropped coverage 1/1/2026 |
| New Jersey | No coverage |
| New Mexico | No coverage |
| New York | No coverage |
| North Carolina | Has coverage* |
| North Dakota | No coverage |
| Ohio | No coverage |
| Oklahoma | No coverage |
| Oregon | No coverage |
| Pennsylvania | Dropped coverage 1/1/2026 |
| Rhode Island | Has coverage |
| South Carolina | Dropped coverage 1/1/2026 |
| South Dakota | No coverage |
| Tennessee | Has coverage |
| Texas | No coverage |
| Utah | Has coverage |
| Vermont | No coverage |
| Virginia | Has coverage |
| Washington | No coverage |
| West Virginia | No coverage |
| Wisconsin | Has coverage |
| Wyoming | No coverage |
States with “Dropped coverage” eliminated GLP-1 weight loss coverage effective January 1, 2026.
*North Carolina dropped coverage in October 2025 due to a state budget stalemate, then reinstated it in December 2025.
Track Health Care Policy
The ever-evolving state health policy landscape will continue to influence how health care organizations make business decisions. MultiState’s team pulls from decades of expertise to help you effectively navigate and engage. MultiState’s team understands the issues, knows the key players and organizations, and we harness that expertise to help our clients effectively navigate and engage on their policy priorities. We offer customized strategic solutions to help you develop and execute a proactive multistate agenda focused on your company’s goals. Learn more about our Health Care Policy Practice.